Medical Emergencies
The following are danger signs which need urgent medical attention. Do not attempt to treat these yourself:
- Any severe injury to the eye
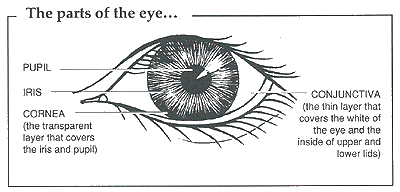
- Any condition in which the vision suddenly becomes severely affected, such as acute glaucoma where the pupil is enlarged and the eye is very hard, or acute iritis where the pupil is small and irregular.
Ideas for a simple ‘Eye Tray’...
- Amethocaine 1% eye drops (anaesthetic drops)
- Sterile fluorescein strips - to show up damage on the eye surface
- Absorbent tissues - for cleaning
- Tetracycline eye ointment – antibiotic
- Epilation forceps - for removing ingrowing eyelashes
- Cotton tips - for cleaning and removing foreign bodies
- Sterile large needles - for removing small foreign bodies on the cornea
- Eye pads, adhesive tape and bandages
- Scissors
- Magnifying glass
- Small focusing torch
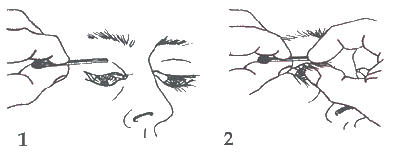
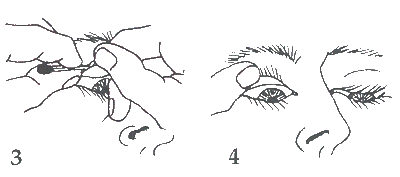
(3). The match stick can then be gently removed and the lid is kept in the everted position by pressing the lashes against the skin. The patient must keep looking down, or the upper lid may flip back.
Either hand can now be used to hold the eyelid in place so the other hand is free to work at removing a foreign body if one is present (4).
Removing a foreign body
If the foreign body is on the conjunctiva, use the corner of a small piece of clean cloth or a piece of clean folded paper to gently lift it off. Or wash it off with clean water. Removing a foreign body from the cornea is more difficult. First try washing it off with clean water. If the foreign body is slightly embedded, it can sometimes be removed with the light touch of some small, sterile instrument. A sterile needle mounted on a 2 ml syringe is often used. The needle is always directed across the eye, never towards the eye.
This is obviously a very delicate operation needing a steady hand. Use good light and a magnifying glass. Insist that the patient fixes their good eye on some nearby object to keep both eyes still. It is safer and kinder to use one drop of anaesthetic in the eye - for example, amethocaine 1% eye drops. A further tip is to steady your hand lightly on the patient’s face or forehead. After successfully removing the foreign body it is wise to put a little antibiotic eye ointment into the eye.
I cannot stress too strongly that this operation should only be attempted if the foreign body is lightly embedded.
If a foreign body is deeply embedded, you could cause great damage. In this case patients must be referred to an eye department.
Chemical injuries
If the eyes have been injured by chemicals - for example acid burns or the even more serious alkali burns such as common lime used in whitewash, or from pesticides - the most important treatment is immediate, thorough washing with plenty of clean water, ideally after two drops of amethocaine 1% to relieve the eyelid spasm. This should be done urgently until all the chemical or particles of lime have been washed out. Then a little antibiotic ointment should be applied and the person referred to an eye department as an emergency.
Blunt injuries
First aid treatment for injuries to the eye with a blunt object is bed rest, a dark cover or shade over both eyes and aspirin. Such cases must be urgently referred for expert help.
Eye infections
Infection of the eyelid margins (blepharitis)
This is an infection (staphylococcal) of the glands around the base of the eyelashes causing pain and swelling. The eyelids have red swollen edges and loose, often irregular lashes. The eyes are irritable, watery and often sensitive to light.
Dirty, unhealthy living conditions, poor personal hygiene, smoke and dust, ill health and seborrhoea (cradle cap) all increase the likelihood of this infection.
Treatment consists of improving general health and treating seborrhoea if this is present. The eyelids should be washed gently and massaged twice a day using a moist cotton-tipped bud (eg: a Q-Tip) to remove scales and discharge. Then tetracycline 1% or sulphacetamide 6% should be rubbed into the lash roots twice a day for a month. If available hydrocortisone may also be used for the first week. In severe cases gentian violet is a useful addition to this treatment - if a bit messy.
Stye (hordeolum)
This is a red swollen lump on the eyelid margin, developing when an eyelash gland becomes infected. Removing the affected lash may speed up recovery. ‘Hot spooning’ three or four times a day will help to speed healing. To do this, wrap a few turns of a bandage around a clean wooden spoon on which you hold some cotton wool. Dip it in hot water; squeeze out the water and apply gently to the eye. When it has cooled repeat the process five to ten times. Apply an antibiotic cream three times a day.
Conjunctivitis
This is an infection of the conjunctiva. There are a number of different causes of conjunctivitis, but all have the same signs and symptoms...
- pain - from mild itching to severe pain
- discharge - may even be pussy, causing eyelids to stick together on waking
- redness - of varying degree
- no change in vision.
We will look at four of the main kinds of conjunctivitis...
Conjunctivitis of the new-born (neonatal conjunctivitis)
If a baby develops conjunctivitis in the first few weeks of life, it has been infected either from the mother during birth or from the hands of birth attendants. Such infections must be treated immediately or the baby may lose its sight. The most usual cause is gonorrhoea from the mother - conjunctivitis develops within a few days.
Treatment is penicillin G given by mouth and antibiotic eye drops. Drops are put into both eyes every five minutes until the discharge stops. This may take an hour or two. Drops are then given at decreasing intervals for about two days.
The best prevention is to wash the eyelids and face of all new-born babies before the eyes are opened. Place an antibiotic ointment in each eye. The use of 1% silver nitrate drops is effective but toxic to the conjunctiva and is no longer used.
Bacterial conjunctivitis (pink eye)
This infection can affect all ages. It begins suddenly in one or both eyes, causing redness, pain and irritation. There is a lot of discharge and lids often stick together after sleep.
This disease is very contagious and easily spreads from one person to another. Do not share towels and always wash after any contact with an infected person. Keep your own face clean because eye-seeking flies help to spread the disease.
Treatment is to wash the eyes with clean water and a cloth as often as necessary. Apply antibiotic ointment - chloramphenicol eye ointment - four times a day.
Trachoma
This is a chronic kind of infection which involves both the conjunctiva and the cornea. It can affect all ages, but particularly young children. It begins with red, watery eyes as with pink eye. A single infection heals without treatment. However, re-infection is very common. After a month or more, small pinkish grey lumps, known as follicles, form in the inflamed conjunctiva of the upper and lower eyelids. The white of the eye (conjunctiva) becomes mildly inflamed. The cornea also becomes scarred and may appear greyish on the top edge due to many tiny new blood vessels (pannus). Eyesight will become affected by pannus.
The end result of severe inflammation in trachoma is a variable amount of scarring of both conjunctiva and cornea, leading to thickened and inflamed lids (entropion) so that vision is progressively reduced.
Trachoma only causes blindness in communities where there is frequent re-infection with chlamydia and other bacteria. Such communities are usually poor, overcrowded, with inadequate sanitation and water supply, poor personal hygiene and many flies.
Individuals can be treated with antibiotics - sulphonamide (eg: triple sulpha) by mouth for three weeks or tetracycline 1% eye ointment (three or four times daily) placed into the eye for six weeks. The acute signs take some months to disappear, but the scarring remains for life.
The real problem is to prevent re-infection and to reduce the overall level of infection within the community. This can be done by the widespread use of tetracycline 1% eye ointment especially, among all school children and pre-school children over a long period of, for example, six months. One good method is to give tetracycline 1% twice daily to all children for one week every month, continued over six months. Together with this, an important and perhaps more practical measure is the daily face washing of all children. So too is the provision of clean water supplies, fly control measures and sanitation. Family planning programmes may help to reduce the population density of small children living together who continually re-infect each other with the disease.
Acute viral conjunctivitis
This may affect all ages. It infects both eyes though it may begin with just one. There is soreness and swelling around the eyes, and some watery discharge. The pain may be mild or severe and, because the cornea is frequently involved, there may be extreme sensitivity to light. Often this kind of conjunctivitis is associated with fever and sore throat.
There is no specific treatment. Dark glasses may help. Chloramphenicol eye ointment is not of much value.
Dr Anderson has worked for many years as an ophthalmologist in Pakistan, Afghanistan, India and Africa, and was until recently senior lecturer in the Department of Preventive Ophthalmology at the Institute of Ophthalmology in London.